These are the UK coronavirus stories you need to know about today.
BMA's Lockdown Exit Strategy
The BMA has issued a strategy document for England's exit from the current lockdown on 3 December.
It says measures are needed to bridge the gap until widespread vaccination.
Recommendations include:
- Reforming Test and Trace with more local involvement
- Replacing the 'rule of six' with a two household rule for social mixing
- Banning travel between different tier levels
- Targeted support for clinically extremely vulnerable people and those from at-risk backgrounds, such as BAME communities
"When the first lockdown ended, there was no coherent plan for keeping COVID-19 at bay." Council Chair Dr Chaand Nagpaul said in a news release.
"As England prepares to exit its second lockdown, it is unthinkable that we make the same mistakes again because this time, the impact will be far worse. It’s reasonable to conclude, that without these measures, the NHS will not be able to cope with caring for even the most critically ill patients."
'Exciting' Vaccine News
UK experts have reacted to more positive data from Pfizer on its COVID-19 vaccine candidate.
In a news release the company said: "Primary efficacy analysis demonstrates the vaccine to be 95% effective against COVID-19 beginning 28 days after the first dose;170 confirmed cases of COVID-19 were evaluated, with 162 observed in the placebo group versus eight in the vaccine group.
"Efficacy was consistent across age, gender, race and ethnicity demographics; observed efficacy in adults over 65 years of age was over 94%."
Professor Trudie Lang, director, The Global Health Network, Nuffield Department of Medicine, University of Oxford, told the Science Media Centre: "Today’s update from Pfizer provides further encouraging news and more detail on the protection against disease that their vaccine is showing from this definitive phase 3 trial. The detail on achieving 94% protection in the elderly participants in the trial is particularly excellent news."
Professor Stephen Evans, professor of pharmacoepidemiology, London School of Hygiene & Tropical Medicine, said the announcement was "very good news indeed".
Ahead of submissions to US and European regulators he said: "We can expect both agencies to conduct a very careful evaluation and we can rely on their conclusions. Relying on a press release is not enough."
Meanwhile, preliminary trial results for the CoronaVac COVID-19 vaccine from the Chinese company Sinovac Biotech have been published in The Lancet Infectious Diseases.
The authors write: "In summary, CoronaVac was well tolerated and induced humoral responses against SARS-CoV-2, which supported the approval of emergency use of CoronaVac in China and in three phase 3 studies. The protective efficacy of CoronaVac remains to be determined."
COVID-19 Legal Protection
The Medical Protection Society (MPS) has written to Boris Johnson calling for legal protection for doctors against criminal or disciplinary action for clinical decisions made amid scarce resources.
MPS Medical Director Dr Rob Hendry wrote: "The moral and emotional burden of effectively choosing who lives or dies should not be placed on the shoulders of frontline staff, not least as they could then be vulnerable to allegations of unlawful killing."
The Guardian quotes a Department of Health and Social Care spokesperson: "New protections during COVID-19 mean that frontline NHS staff and hospitals can focus on treating patients with greater confidence and ensure that patients have access to redress if things go wrong."
First Wave Capacity
Thirty percent of England's hospitals reached maximum capacity for ventilator beds at some stage in the first wave, according to preprint University of Warwick led research.
Uneven distribution of resources meant that Nightingale field hospitals were often underutilised.
Dr John Dennis, research fellow at the University of Exeter Medical School, commented: "Our study shows the potential benefit of using real-time information to inform management of hospitals during the second-wave of the pandemic, and making this information available locally, regionally, and nationally. Doing so could enable hospitals to maintain safe occupancy levels and can provide the best possible care for patients."
PPE Procurement Report
The National Audit Office has published a report on the Government's £18b PPE contracts. Companies recommended by MPs, peers, and advisers were given priority to win government contracts, it said.
It found "specific examples where there is insufficient documentation on key decisions, or how risks such as perceived or actual conflicts of interest have been identified or managed. In addition, a number of contracts were awarded retrospectively, or have not been published in a timely manner. This has diminished public transparency, and the lack of adequate documentation means we cannot give assurance that government has adequately mitigated the increased risks arising from emergency procurement or applied appropriate commercial practices in all cases. While we recognise that these were exceptional circumstances, there are standards that the public sector will always need to apply if it is to maintain public trust."
Sky News reported Cabinet Office minister Julia Lopez's comments: "As this report rightly recognises, we needed to procure contracts with extreme urgency to secure the vital supplies required to protect frontline NHS workers and the public and we make no apology for that.
"We have robust processes in place for spending public money to ensure we get critical equipment to where it needs to go as quickly as possible, whilst also ensuring value for money for the taxpayer."
Self-isolating
Boris Johnson took Prime Ministers' Questions remotely today. He's still self-isolating in Downing Street after being 'pinged' by Test and Trace. He tested negative with a rapid turnaround lateral flow test.
Head of England's Test and Trace, Baroness Dido Harding, is isolating after getting an alert from the tracking app.
Also self-isolating is NHS England Medical Director Professor Stephen Powis after a family member tested positive.
He took part in a Downing Street news briefing remotely and presented the latest data, including on hospital admissions.
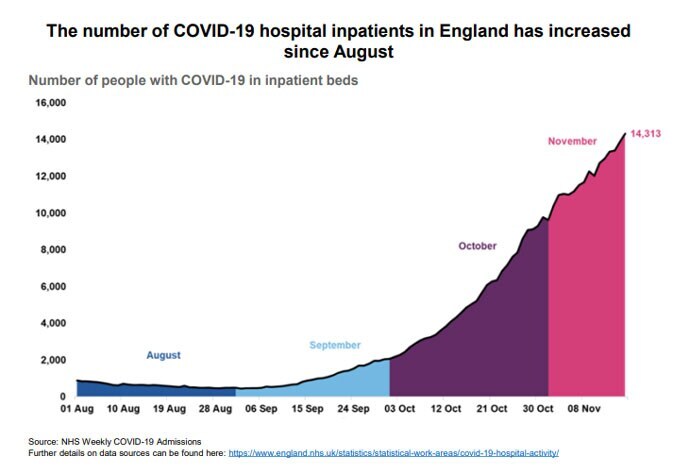
In today's daily data another 19,609 UK positive tests were reported and 529 deaths.
There are 16,271 COVID-19 patients in hospital and 1420 ventilator beds are in use.
Pandemic 'Catalyst for Change'
The pandemic should be a catalyst for change, according to GMC Chair Dame Clare Marx in a speech to the Leaders in Healthcare conference.
"Environments that promote collaboration, communication, and accessible leadership produce better outcomes," she said. "Environments where those factors are absent are, at best, unpleasant to work in and, at worst, downright dangerous."
She said new research to be published early next year will show more than 35% said dissatisfaction with their working environment was a reason for leaving medicine, and 25% said it was a reason they did not want to return.
Lockdown Binge Drinking
More than four million over 50s in the UK are binge drinking at least once a week under lockdown, according to new polling of 1150 adults earlier this month.
Julie Breslin from the drug, alcohol, and mental health charity With You commented: "Many older adults are unable to see their loved ones or friends and are drinking more as a way to cope with increased loneliness, isolation, and anxiety. As people age their bodies find it harder to process alcohol, so the number of people over 50 who are binge drinking at the current time is really alarming. The impact of this will ripple through families as well as support services and the NHS."
Airline Testing
BA and American Airlines have begun a free COVID testing trial for transatlantic passengers to help gather evidence for shorter self-isolation periods.
The first remotely supervised home test is done 72 hours before departure from the US.
A LAMP test is done on arrival at Heathrow and a home test kit is issued to be used 3 days later.
BA Chief Executive Sean Doyle said in a statement:"We need the UK Government to introduce a system that allows travellers to take reliable, affordable tests before departure, so they are confident that fellow passengers are COVID-free. For people arriving from countries with high infection rates, a further test on arrival should then release them from quarantine."
Open a Window
The importance of ventilation is the subject of the latest Government public information campaign.
GP Dr Amir Khan said: "Fresh air is extremely beneficial. For COVID-19, it is important to ventilate indoor spaces if someone in your home has the virus as this can help prevent transmission to other household members.
"You should also let fresh air into your home when you have any visitors and just after they leave in case they are infected."
See more global coronavirus updates in Medscape’s Coronavirus Resource Centre.




