Following the death of six-month-old Noah Thahane from complications of vitamin D deficiency, clinicians and academics at the University of Birmingham are calling for the introduction of mandatory primary care-based monitoring of vitamin D levels in babies and pregnant women.
Noah Thahane, of African descent, suffered a fatal cardiac arrest at home. Post-mortem examination revealed that he had severe rickets and complications associated with vitamin D deficiency. While his mother had received antenatal multivitamin supplementation and attended all postnatal child surveillance and vaccination appointments, she was not informed of the need for infant vitamin D supplementation.
A six-month-old boy of Somalian heritage and a five-month old British Pakistani girl also presented acutely with cardiac arrest, respiratory arrest following seizure or severe respiratory distress, with profound hypocalcaemia (1.22-1.96mmol/L).
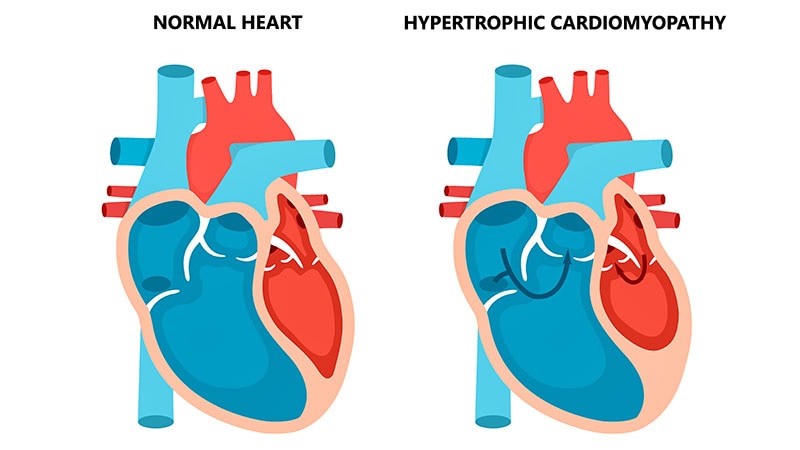
All three had severely dilated left ventricles with reduced ejection fraction, fractional shortening and global hypokinesia, confirming hypocalcaemic dilated cardiomyopathy.
The authors of the case presentation, published in BMC Pediatrics, say Noah’s death was “entirely preventable”. They are calling on the Government to introduce mandatory monitoring of babies and pregnant women and to ensure vitamin D supplements are being used when necessary.
They also recommend that studies should explore the feasibility of introducing a rickets prevention programme which would see children receiving oral bolus vitamin D supplements alongside routine immunisations at GP surgeries, with a similar strategy for pregnant women at antenatal visits.
“The severe, hidden, cardiac and bone pathology described here exposes a failure of public health prevention programmes, as complications from vitamin D deficiency are entirely preventable by routine supplementation. The family investigations demonstrate widespread deficiency and undiagnosed osteomalacia in ethnic risk groups and call for protective legislation,” they say.